Clove Oil: A Natural Remedy for Bleeding Gums You Need to Try
Bleeding gums, a common symptom often associated with gingivitis and periodontitis, can significantly impact oral health and overall well-being. While conventional treatments exist, many individuals seek natural alternatives to address this issue. Clove oil, derived from the dried flower buds of the Syzygium aromaticum tree, has emerged as a promising natural remedy due to its potent antimicrobial and anti-inflammatory properties. This article delves into the efficacy of clove oil in treating bleeding gums, exploring its mechanisms of action, supporting evidence, usage methods, potential side effects, and important considerations.
Understanding the Etiology of Bleeding Gums
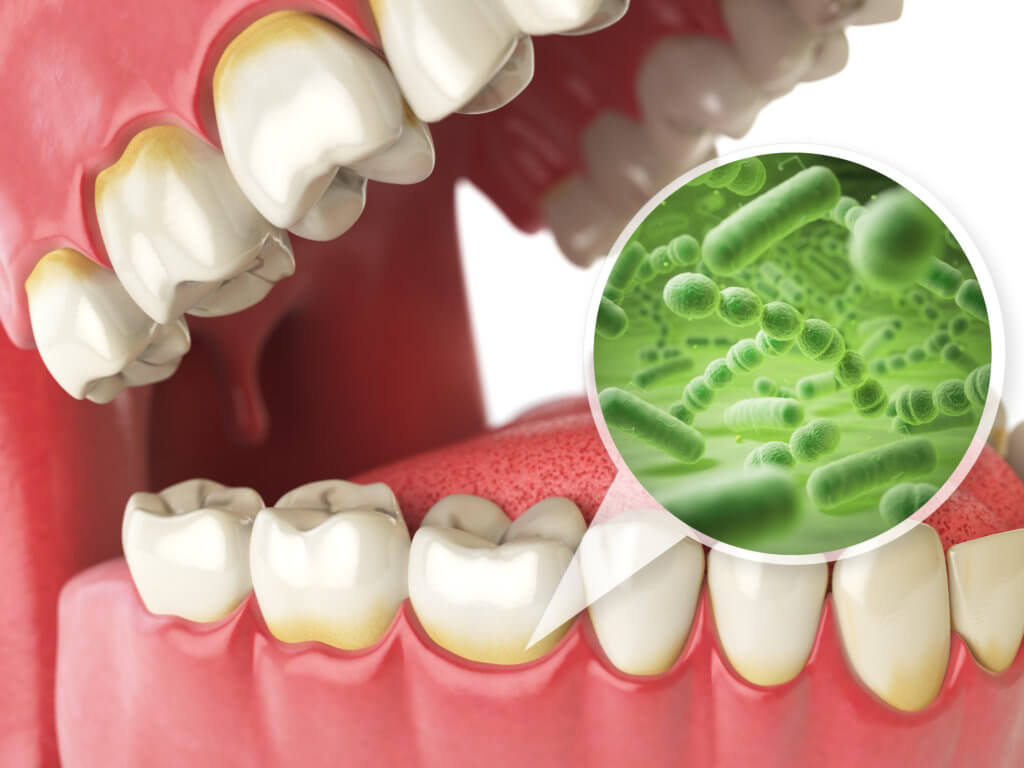
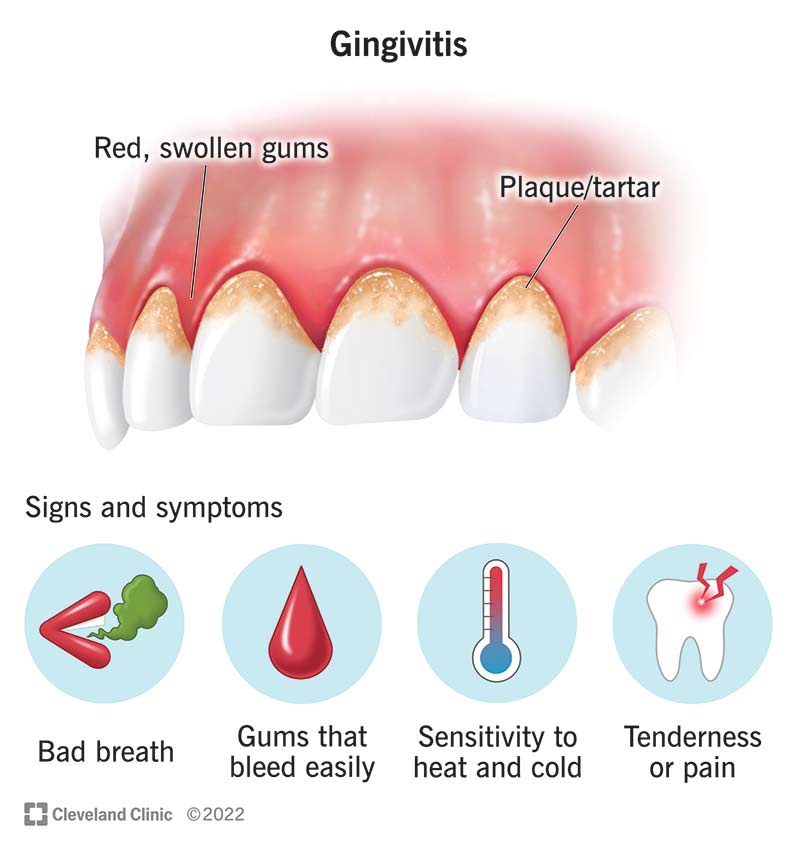
Bleeding gums, medically termed gingival bleeding, are primarily a consequence of gum inflammation, a condition often triggered by poor oral hygiene. Gingivitis, the initial stage of gum disease, is characterized by inflamed and swollen gums that easily bleed. This inflammation is a direct response to the bacterial biofilm (plaque) that accumulates on the teeth and gum line. If left untreated, gingivitis can progress to periodontitis, a more severe form of gum disease that involves the destruction of the supporting tissues and bone surrounding the teeth, potentially leading to tooth loss.
Several factors contribute to the development of bleeding gums, including:
- Insufficient oral hygiene practices, such as infrequent brushing and flossing.
- Hormonal changes, particularly during pregnancy or menopause.
- Certain medical conditions, such as diabetes and leukemia.
- Genetic predisposition to gum disease.
- Smoking and tobacco use.
- Nutritional deficiencies.
- Medications with side effects that affect gum health.
Addressing the underlying cause of bleeding gums is crucial for effective treatment. While clove oil can provide symptomatic relief, it should not replace regular dental checkups and professional oral hygiene maintenance.
Clove Oil: A Comprehensive Overview of its Properties
Clove oil's therapeutic potential stems from its rich composition of bioactive compounds, most notably eugenol. Eugenol constitutes a significant portion (up to 90%) of clove oil's composition and is responsible for many of its beneficial effects. This potent phenolic compound possesses remarkable antimicrobial, anti-inflammatory, and analgesic properties.
Antimicrobial Action
Eugenol exhibits broad-spectrum antimicrobial activity against a wide range of bacteria, fungi, and viruses commonly implicated in oral infections. Its ability to disrupt bacterial cell membranes and inhibit their growth makes it effective in combating the pathogens associated with gingivitis and periodontitis. Numerous studies have demonstrated clove oil's effectiveness in reducing bacterial load in the oral cavity.
Anti-inflammatory Effects
Inflammation plays a central role in the pathogenesis of bleeding gums. Eugenol's anti-inflammatory properties help to reduce gum swelling and bleeding by modulating the inflammatory response. It achieves this by inhibiting the production of pro-inflammatory mediators, thereby alleviating the symptoms of gingivitis.
Analgesic Properties
Clove oil's analgesic properties provide pain relief, which is particularly beneficial for individuals experiencing discomfort associated with inflamed gums. This pain-relieving effect further enhances its therapeutic value in managing bleeding gums.
Scientific Evidence Supporting the Use of Clove Oil
While research on clove oil's efficacy in treating bleeding gums is ongoing, several studies have demonstrated its promising therapeutic potential. Many in vitro studies have confirmed clove oil's potent antimicrobial and anti-inflammatory effects against oral pathogens. Furthermore, preliminary clinical trials have shown encouraging results in reducing gingivitis symptoms, including bleeding gums, when used as a mouth rinse or topical application.
However, it's crucial to note that the existing research base is limited, and more large-scale, rigorously designed clinical trials are needed to definitively establish clove oil's efficacy and optimal dosage for managing bleeding gums. The results observed in these studies need to be corroborated by larger, more controlled studies to provide definitive conclusions.
Methods of Using Clove Oil for Bleeding Gums
Clove oil can be used in several ways to address bleeding gums:
- Mouth rinse: Dilute a few drops of clove oil in a glass of water and use it as a mouth rinse for 30-60 seconds, then spit it out. Caution: Never swallow clove oil.
- Topical application: Apply a small amount of diluted clove oil directly to the affected gum area using a cotton swab. Ensure that the oil is properly diluted to avoid irritation.
- Toothpaste addition: A small amount of clove oil can be added to your regular toothpaste. This is another method to improve oral health. However, it is important to note that it should not substitute for effective brushing and flossing.
It's imperative to dilute clove oil before application, as undiluted clove oil can cause irritation and burning sensations. A typical dilution ratio is 1-2 drops of clove oil per ounce of water or carrier oil (such as coconut oil).
Potential Side Effects and Precautions
While generally safe when used appropriately, clove oil can cause certain side effects in some individuals. These include:
- Allergic reactions: Individuals allergic to clove or eugenol may experience skin irritation, itching, or swelling. A patch test is recommended before widespread use.
- Mouth irritation: Undiluted clove oil can cause burning or irritation of the gums and oral mucosa.
- Gastrointestinal upset: Ingesting clove oil can lead to nausea, vomiting, or diarrhea. Therefore, it’s important to avoid swallowing the oil.
- Interactions with medications: Clove oil may interact with certain medications, such as blood thinners. Consult your doctor or dentist before using clove oil if you are taking any medications.
Pregnant and breastfeeding women should consult their healthcare provider before using clove oil. Children should also only use clove oil under the guidance of a dentist or physician.
Conclusion
Clove oil presents a promising natural remedy for bleeding gums due to its potent antimicrobial and anti-inflammatory properties. However, it is crucial to use it cautiously, diluting it appropriately to avoid irritation and potential side effects. While preliminary evidence supports its efficacy, more robust clinical trials are needed to fully elucidate its therapeutic potential. Clove oil should be considered a complementary therapy and not a replacement for professional dental care. Regular dental checkups, proper oral hygiene practices, and addressing any underlying medical conditions remain essential for maintaining optimal oral health and preventing the progression of gum disease.